Published: Saturday, May 18, 2020
Editor’s Notes
This article has been reviewed by Science X.
Editorial process
Policies.
Editors have highlighted
The content must have the following attributes to ensure its credibility:
fact-checked
Trusted source
Written by a researcher
Proofread
The Conversation, Justin Stebbing
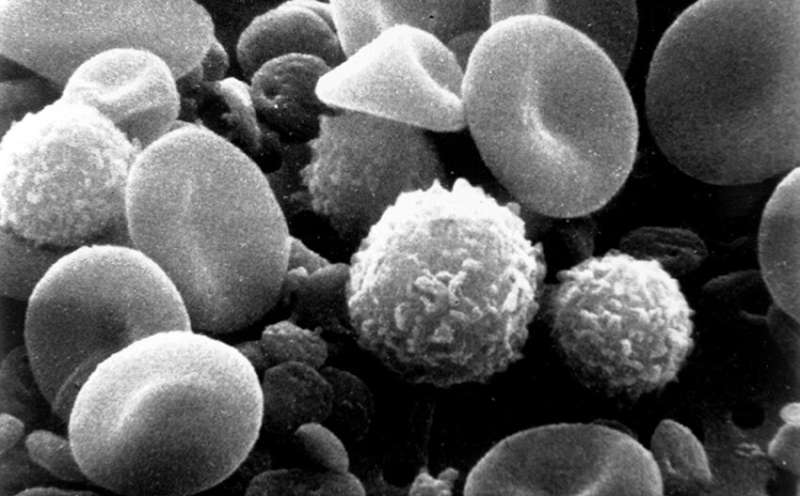
Credit: National Cancer Institute. An electron micrograph of blood showing myeloid immune cells and red blood cells. Credit: National Cancer Institute
The immune system is a complex defense network that can identify and neutralize threats. The immune system is a protector, patrolling the body constantly to protect it from intruders such as bacteria, viruses and cancer cells.
Immunotherapy is revolutionizing medical treatment by harnessing the body’s own defense mechanisms. It boosts, redirects or restores your body’s immune system to eliminate abnormal cells such as those that cause cancer or autoimmune diseases.
However, immunotherapy is costly. Chemotherapy and radiation therapy remain the most common cancer treatments. These conventional methods may damage both healthy tissue and abnormal cells. These methods can also have side effects that are debilitating, including nausea, vomiting and fatigue.
Immunotherapy is a treatment that uses the body’s own immune system to fight diseases. It does so with minimal harm, by blocking checkpoint inhibitors (PD-L1 and CTLA-4), which cancer cells use to shut down the immune systems.
Checkpoint inhibitors were awarded the Nobel Prize for their discovery, and are now widely used in immunotherapy. They block surface proteins which prevent immune cells attacking cancer cells. These inhibitors work by releasing the body’s own natural defense against cancer.
Tumors that are both hot and cold
According to their interaction with the immunity system, tumors are classified as “hot” and “cold”.
Hot tumors exhibit a strong immune response. Infiltrating immune cell engage actively with cancer cells. Cold tumors, on the other hand, show minimal immune activity and are often undetected by the immune system.
Immunotherapy is effective in tumors that are hot, such as lung cancers, kidney cancers and melanoma. Many tumors, such as colon cancers and other types of cancers, do not respond well to immunotherapy. This is because they are able to avoid immune surveillance.
Immunotherapies, which include those that target cold tumors, are now being developed and could benefit more cancer patients. Combination therapies that combine more effective immune checkpoint inhibitors with other agents such as chemotherapy and drugs currently in trials can be used to prime the immune response and enhance tumor recognition.
Other approaches are also available.
CAR-T Cell Therapy
CAR-T cells are extracted from a patient and genetically engineered to produce chimeric receptors, proteins on the surface that detect cancer. The cells are then reintroduced into the bloodstream. Once inside the human body, the modified cells of the immune system target and destroy cancerous cells. The treatment was initially used for tumors like leukemias or lymphomas, but is now being applied to other types of cancer.
Natural killer cells with a variable phenotype
In a 2024 study, “invariant killer cells,” which coordinate the immune response of the body, were used as immunotherapy in cases of severe infections. This was when people with a viral infection on their lungs couldn’t breathe. The trial showed that patients who were critically ill recovered.
Cancer vaccines, unlike traditional vaccines which prevent infectious diseases and stimulate the immune system’s recognition of cancer cells to attack them. Cancer vaccines can contain antigens, tumor-specific markers or genetic material that trains the immune system to target cancerous cell.
Immunotherapy is a form of truly personalized medicine. For example, there are data on cancer vaccines based on clinical trials that take into account the mutations or changes in a patient’s tumor.
Cancer treatment has many benefits.
Immunotherapy is widely recognized for its effectiveness in treating cancer, but its application could go beyond oncology. Immunotherapy harnesses the immune system’s ability to differentiate self from non-self in order to combat a wide range of illnesses.
Researchers are examining its potential to treat autoimmune diseases, allergies, infectious diseases and neurological conditions such as Alzheimer’s.
Not everyone responds to treatment. Some people resist treatment for reasons that we do not fully understand. The side effects of immunotherapy are not free either. Autoimmune complications include inflammation of the colon and lungs. Immunotherapy is expensive and can be prohibitive for some patients. The uptake of immunotherapy is also limited by the patient selection. Choosing who will benefit most from this treatment, and developing personalized treatment plans remain crucial for maximising results.
Research into immunotherapy is ongoing and could lead to a new era of tailored, targeted treatments. Oncolytic viruses, which can directly attack cancer, and microbiome modulation, in which bacteria are used to increase the activity of checkpoint inhibitors, are examples.
Immunotherapy, as our understanding of immunology deepens and technology advances further, could offer precision medicine for previously incurable diseases. The challenge is making it accessible and available to more patients.
This article was republished by The Conversation under the Creative Commons License. The original article can be read.![]()
Source: Medical Xpress



































